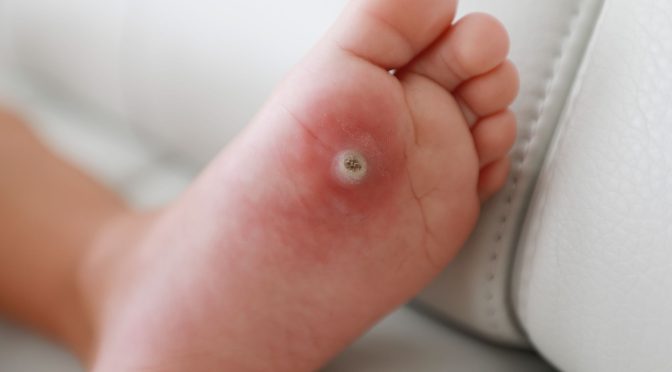
Diabetic foot ulcers and venous leg ulcers are more than just small wounds on the feet and ankles; they’re warning signs of underlying nerve or circulation problems that can lead to serious complications if left untreated. Fortunately, this can be avoided if you know what to look for. Here are the signs of diabetic and venous ulcers and why you shouldn’t ignore them:
Pain, Tingling, Numbness
Many people with diabetes have diabetic neuropathy due to high blood sugar, which causes damage to the nerves, including those in the feet. This often leads to a loss of sensation in the feet. While some people may feel pain as a sign of diabetic foot ulcers, those with diabetic neuropathy won’t feel pain but may experience numbness.
On the other hand, pain is a common sign of venous leg ulcers. Pain can be dull, sharp, throbbing or even burning. Some report that their leg feels heavy or that they feel an itching or tingling sensation. Pain from venous ulcers can range from mild to severe, depending on the stage of the wound.
Redness or Discoloration
Discoloration in the feet, ankles or lower legs is a sign of changes in the skin tissue. For those with diabetes, pink or red discoloration can indicate the beginning of an ulcer formation. The further along diabetic ulcers are, the darker the color usually becomes. Brown, purple or black discoloration usually means a lack of blood flow in diabetic ulcers at more severe stages. For venous leg ulcers, the base of the ulcer is usually red and may have yellow tissue surrounding it. The skin around the ulcer can be reddish brown or purple due to blood pooling in the area.
Swelling in the Feet, Ankles, or Legs
Swelling is a common sign of both diabetic ulcers and venous leg ulcers, although they take slightly different forms. Swelling in diabetic ulcers usually happens in the feet, around the ulcer, while swelling in venous leg ulcers can affect the entire lower leg, the ankle and even down into the foot. If you notice swelling in the legs, feet or ankles that doesn’t improve with rest and elevation, it’s time to get it checked out by a foot and ankle specialist.
Changes in Skin Temperature or Texture
If skin is warm or hot to the touch, this is a sign of inflammation or infection, while cool spots on the skin can indicate poor blood flow. For people with diabetes, the skin in the feet can become dry, callused and scaly. For those with venous disease, the skin in the legs can feel tight and have a shiny appearance. Temperature and texture changes in the skin are both signs that the skin is under stress for one reason or another, making them signs that an ulcer is forming or has already formed.
Slow-Healing Cuts, Blisters, or Sores
In diabetic and venous conditions, the body’s natural healing process is slowed greatly, increasing the risk of infection for even the smallest of cuts, blisters or sores. These small injuries lead to ulcers if they’re not managed properly. Small cuts or sores that don’t heal on their own within a week should be evaluated and treated by a podiatrist because they could be an early sign of forming ulcers.
Why Early Detection Matters
Catching the signs of diabetic and venous ulcers early can make all the difference in the healing process. Prompt treatment and wound care can prevent these wounds from worsening, becoming infected, or possibly leading to extensive treatment and recovery. If you notice any indications of diabetic foot ulcers or venous leg ulcers, including signs of infection like swelling and discharge, reach out to a podiatrist. The team at North Texas Foot & Ankle specializes in providing wound care for any foot and ankle condition. Give us a call at (214) 574-9255 or book an appointment online.